PhD project: Olfactory brain networks determined by DTI and an evaluation of clinical testing tools
Alexander Fjældstad, May 2016
Main supervisor: Therese Ovesen, MD, DMSc, Professor
Supervisor: Arne Møller, MD, Associate Professor
All living creatures depend on their senses to comprehend and interact with the world around us. While a loss of vision, touch, or hearing would result in an immediate clinical workup in the Danish healthcare system, a loss of taste or smell does not elicit any possibility for a clinical examination. Though a gradual loss or complete loss of the sense of smell (i.e. hyposmia or anosmia) can occur relatively unnoticed in many patients, the loss of perceptive capacity will result in a decreased quality of life. However, the main reason why olfactory research has expanded rapidly during the last two decades, is the close relationship between anosmia and brain disease; hyposmia/anosmia has been identified as a prodromal symptom of Parkinson’s disease, it is a strong predictor for cognitive decline in Alzheimer’s, and is closely related to depression.
In a clinical setting, it can be difficult to differentiate central from peripheral etiologies, and identify the underlying pathology. In patients presenting with anosmia in otorhinolaryngological clinics, approximately 70 % are caused sinonasal causes (i.e. chronic rhinosinositis, allergies, or respiratory causes), 10 % are due to post-infectious inflammation of the mucosa, 1 % have congenital anosmia, while the rest will have a central cause for their anosmia (i.e. trauma, tumors, toxicity, psychiatric, neurodegenerative or have another neurologic etiology).
The most widely used smell identification test is the Sniffin’ Sticks (Burghart Messtechnik GmbH, Wedel, Germany) - a psychophysical test to determine olfactory capabilities. The Sniffin’ Sticks can be used as a rapid screening to identify patients in need of an additional diagnostic evaluation. In order to conduct olfactory testing in Denmark, the first phase of the PhD study involved validating and modifying the Sniffin’ Sticks 12-identification test (SIT-12) in an adult Danish population. This allows us to identify and diagnose anosmia, but does not solve the problem of differentiating central from peripheral causes of anosmia.

Figure 1: The Sniffin’ Sticks 12-identification test (SIT-12) can be used to identify anosmic patients, who should undergo further clinical otorhinolaryngologic evaluation.
While MRI scans can unveil brain tumors, the activation of olfactory brain regions in fMRI scans varies widely depending on intra- and inter-individual hedonic value, hunger state, receptor satiation and flow of odorants through the nose. The main study of this PhD is to produce a template of structural olfactory connectivity, as this is not as vulnerable to fluctuations compared with functional olfactory imaging. The first focus is to create this template for normosmic individuals, which will later be tested on anosmic patients suffering from different underlying pathologies to identify characteristic changes in the structural olfactory connectivity network.
The study is conducted at Aarhus University and at University of Oxford.
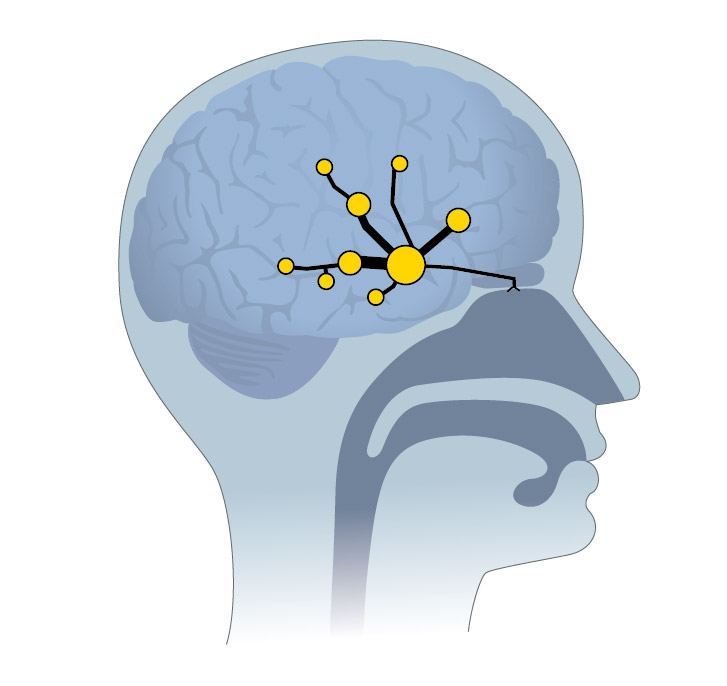
Figure 2: The structural olfactory connectivity network can be evaluated with DTI-scans and the connections in the normosmic adult brain has a homogeneous pattern of connectivity.